

Dialysis can no longer be business as usual. While many may feel that we live in a post-pandemic society, we have data to suggest otherwise, as there have been spikes across the nation, mostly from a combination of the unvaccinated and the highly contagious delta variant.
As of 2018, 786,000 people in the U.S. were living with end-stage renal disease, known as ESRD for short. About 80% of ESRD patients are 65 or older. Coincidentally, the 65 and older group is also the most vulnerable when it comes to the effects of coronavirus.
While some ESRD patients are lucky enough to receive a functioning kidney transplant, 70% of patients with ESRD must undergo dialysis to stay alive and healthy. Despite the statistics, large dialysis providers center their designs around the needs of active, middle-aged dialysis patients. By making the overwhelming majority of hemodialysis treatment available only at outpatient clinics, providers put nursing home residents in a risky, inconvenient position.
The limits of outpatient providers
Outpatient treatment poses infection risk to everyone involved. The dialysis patients themselves, the staff and other nursing home residents are all exposed to pathogens dialysis patients carry back from outpatient clinics every few days. Traveling to a dialysis clinic, especially for residents who can’t transport themselves, poses a whole array of challenges. For the resident, the ride is disruptive, confusing and time-consuming. For nursing home operators, providing ambulance transportation for outpatient dialysis may cost them up to $411 per round trip.
Finally, not every nursing home resident can be seen by an outpatient clinic. Highly acute residents struggle to find placement at outpatient clinics even in normal times. With a pandemic, their severe health conditions put them even more at risk.
A few hours saved can make a world of difference
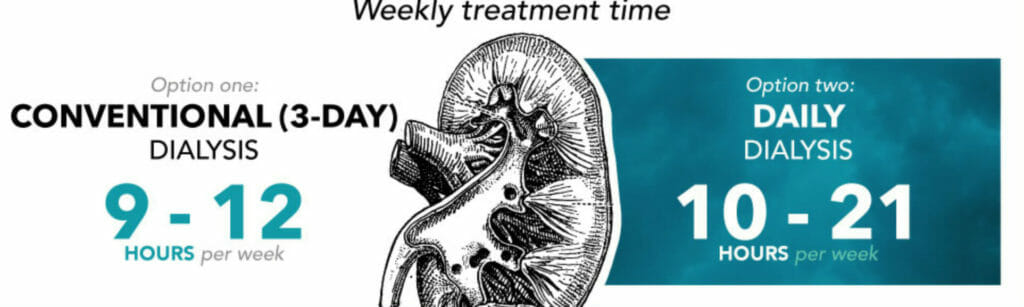
Home hemodialysis limits the risk of multiple visits outside one’s green zone. When you compare the weekly treatment times, the conventional three-day dialysis comes out to nine to 12 hours per week, whereas daily dialysis is 10 to 21 hours per week. Converting a nursing home population to three-day dialysis not only cuts down the treatment time by 17% but also eliminates hours of travel time. This decreases the risk of infection and complications and also allows nursing home staff to repurpose this would-be lost time for other therapies and social activities.
More than stopping the spread of coronavirus variants, on-site dialysis is at the forefront of clinical innovation. The change in location allows for better collaboration of care, fewer hospital readmissions and stronger relationships between nursing home operators and hospital partners.
Three-day dialysis is preferable to daily because not many residents would have to make changes. About 98% of nursing home dialysis patients are already accustomed to three-day out-patient dialysis. Switching them to daily treatment would require prescription changes. Bringing such changes about may cause confusion and disrupt continuity of care.
Three-day dialysis is also safer for residents than daily dialysis. Daily dialysis has more chances of potentially leading to hospitalization or surgery. Complications with higher risks from daily dialysis include difficulty with the blood-access site, blood clots and aneurysms. More frequent treatment also increases the odds of a resident missing treatment one day, which can have severe consequences.
While quality of care is a nursing home’s top priority, all institutions must take the cost of their services into account. Here again, three-day dialysis is a better alternative than daily dialysis. For the same initial investment, on-site, three-day dialysis provides treatment to three times more patients than daily dialysis. Imagine a facility has six chairs specially made for dialysis treatment. Three-day dialysis in six chairs can support up to 36 patients. Meanwhile, daily dialysis would only support 12 in the same conditions.
A changing industry
Large dialysis providers have failed to deliver effective and flexible treatment for nursing home patients, thereby highlighting the need for a new model. That model is in-house dialysis care designed for geriatric patients. This level of at-home care allows caregivers to embrace all patient comorbidities and work around additional risks on a more personal level. Close collaboration with a skilled nursing facility team can ensure continuity of care, generate customized care plans for unique patients and offer nursing, nutritional and psycho-social care combined.
“Forward-looking operators are increasingly embracing the value of onsite dialysis services. Destination facilities – especially those seeking to attract higher acuity patients – understand that a SNF can distinguish itself when it’s able to meet the patients where they are,” says Shimmy Meystel, CEO, Concerto Renal Services. “For patients requiring kidney care, that means offering 3-day weekly onsite dialysis. It’s a win for residents and operators alike, with transportation risks and costs erased and better collaboration of renal care. And best of all, it acts as infection disease insurance against COVID and other pathogens.”
Brian Wallace is the founder and president of NowSourcing, an industry leading content marketing agency that makes the world’s ideas simple, visual and influential. Brian has been named a Google Small Business Advisor for 2016-present and joined the SXSW Advisory Board in 2019-present.
The opinions expressed in McKnight’s Long-Term Care News guest submissions are the author’s and are not necessarily those of McKnight’s Long-Term Care News or its editors.





