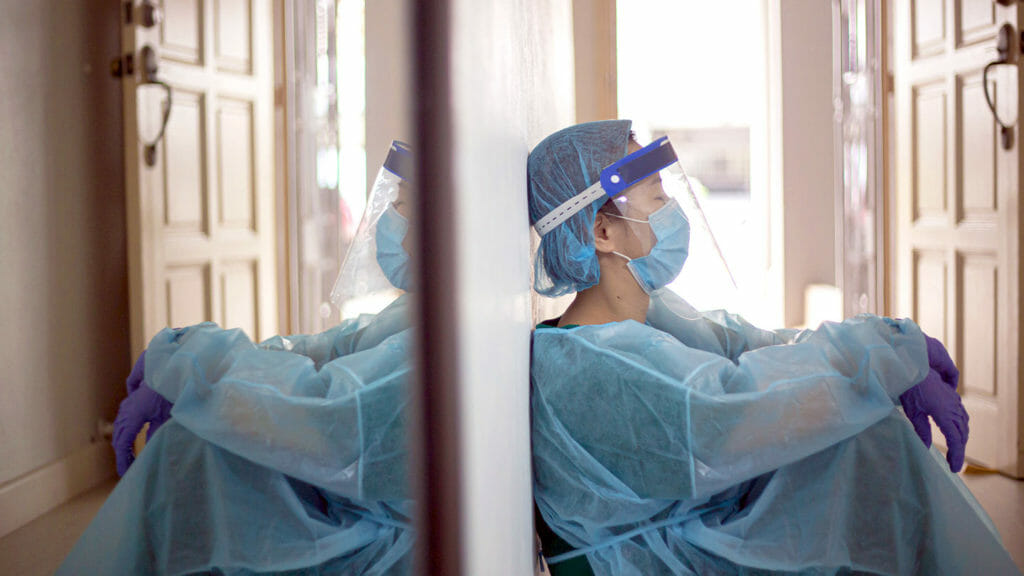
For months, provider organizations have been bemoaning the costs of relying on temporary staff that eat up limited, taxpayer-supported Medicare and Medicaid dollars.
But nationwide, there’s one set of nursing homes feeling a unique pain associated with being short-staffed and unable to recruit in this tight labor market: Those owned by the taxpayers themselves.
County-run and other municipal-owned nursing homes are struggling mightily with public budget issues that limit the options for wage increases and slow the processes needed to address urgent hiring and retention challenges.
In New Hampshire, for example, the Belknap County Board of Commissioners last week scheduled an emergency meeting to discuss how it can raise wages at its 94-bed nursing home, and whether it will be possible to bring in National Guard members to deliver patient care.
Commission Chairman Peter Spanos has said Belknap County Nursing Home is in “crisis mode.” County leaders said the facility has been losing nurses to other local long-term care facilities that can pay substantially more — sometimes twice as much. While the county recently hired three travel nurses for a three-month period, officials plan to discuss other ways to address the staffing shortage today.
“We are going to discuss whether or not we can do a lump-sum payment or significantly adjust wages,” County Administrator Debra Shackett told local media last week.
The number of county-owned facilities is dwindling across the United States. In Pennsylvania, for example, there were 16 operating in 2021, just 44% of the 36 in 2004. Yet in rural and underserved communities, they remain an especially important care option for elderly residents.
Belknap County’s Spanos said wages at that nursing home have been “artificially low for many, many years” and that other county nursing homes in New Hampshire face similar hurdles.
Often, municipal bodies need to seek approval through their local funding hierarchy before reallocating funds in support of wage or benefit changes or operational overhauls that might give workers more flexibility. Pay raises given to workers in one municipal setting also can affect pay for other classes of workers, and many state- and county-owned facilities also have union contracts to consider.
COVID-19 and vaccination mandates also play a role.
Nursing home workers have pursued lawsuits against municipalities that enacted vaccine mandates of their own, and others have threatened to walk off their government jobs as the federal rule covering healthcare workers approaches.
Also in New Hampshire, leaders of the county-owned Maplewood Nursing Home leaders predicted they could lose a dozen of roughly 250 employees due to the federal mandate. The home plans to close its third floor and move those residents to available beds on the second and fourth floors in early December, Administrator Kathryn Kindopp told The Sentinel last week.
Belknap, meanwhile, has been operating at two-thirds capacity because of the staff shortage. Nursing home Administrator Shelley Richardson told commissioners she hopes whatever proposal for higher wages the commission supports will be sufficient to stabilize staffing so the nursing home will be able to stay open for the rest of this year “and hopefully well into 2022.”




