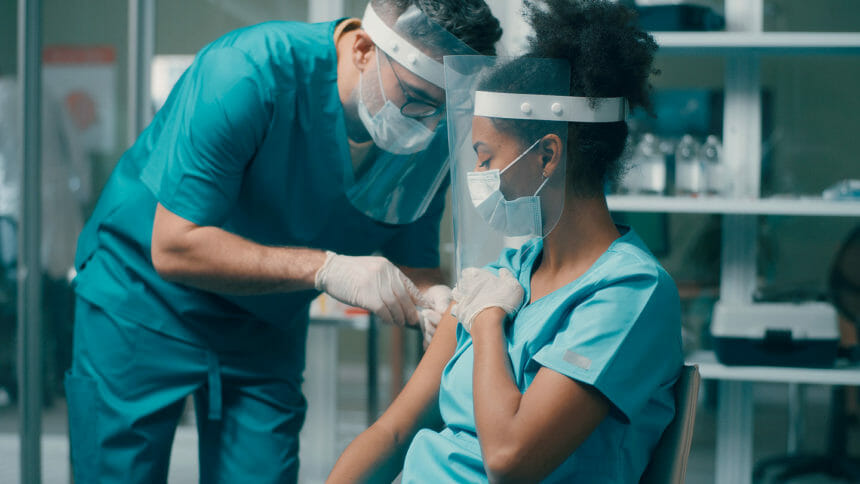
A major COVID-19 vaccine mandate deadline for nursing home workers hit Tuesday, and it did so without the major exodus of employees that many had warned would further threaten the staff-depleted industry.
Many stakeholders told McKnight’s Long-Term Care News on Tuesday that vaccine literacy was a key why massive losses due to the mandate have been avoided.
“Our focus from the very beginning has been on education. We have an ongoing extensive education campaign where we offer explanation and interpretation of the latest orders, directives and guidance related to the coronavirus pandemic, in addition to providing general information and resources,” Nick Van Der Linden, director of communications for LeadingAge Florida, explained.
“As part of that campaign, we focused on understanding vaccination hesitancy and how our members could educate their staff about the safety and benefits of being vaccinated,” he added.
Surveyor instructions
The second big deadline to have healthcare workers vaccinated, or exempt, hit Tuesday for the 24 states that unsuccessfully challenged the rule in federal court and the start of enforcement actions by the Centers for Medicare & Medicaid Services. That leaves only Texas to hit a final deadline for having both shots.
A CMS spokesman on Tuesday told McKnight’s the agency’s main focus is to bring healthcare providers and suppliers into compliance. That’s why it will assess the severity of any failures to meet these standards and work with providers to get them back on track before pursuing stronger enforcement measures such as exclusion from the Medicare or Medicaid programs.
Enforcement of the staff vaccination requirement is currently underway nationwide as a part of complaint and standard recertification surveys, the spokesman said. If found non-compliant, CMS will use civil monetary penalties and perhaps denial of payment before termination from the Medicare and Medicaid program as a final measure.
“While onsite, surveyors will review the healthcare provider’s COVID-19 vaccination policies and procedures, the number of resident and staff COVID-19 cases over the last four weeks, and a list of all staff and their vaccination status,” the spokesman said. “This information, in addition to interviews and observations, will be used to determine the compliance of the provider or supplier with these requirements.”
Watchdog on the prowl
The Office of the Inspector General is also launching an investigation this year to see if compliance was actually achieved by providers by the final deadline.
Currently, about 85% of nursing home staff have been vaccinated nationwide. For Florida, that figure is about 89% even though exemptions have played only a small role in the figure, according to Van Der Linden. He noted that previous, self-imposed mandates helped providers in the state reach their targets.
“We’ve seen great success with that and feel comfortable with our members’ abilities to comply with the CMS deadlines,” he said.
Exemptions’ big role
There were two main reasons providers haven’t seen a mass exodus of non-vaxing employees, said Dave Voepel, president and CEO of the Arizona Health Care Association, to McKnight’s on Tuesday, when his members were subject to their second-shot deadline.
First, he believes pandemic fears and uncertainty shook out thousands of employees nationwide before any vaccine mandates were set.
Second, he estimated that facilities statewide have granted exemptions — mostly religious — to about 15% to 20% of the workforce. This has enabled providers to clear Centers for Medicare & Medicaid Services thresholds and account for virtually 100% of staff.
“We weren’t bad originally because we had Banner Health, the state’s largest employer with about 46,000 workers, which did a vaccine mandate on its own, even before CMS announced its,” Voepel said. “That alleviated some of the issues.
“If it weren’t for the exemptions, we would not be able to make it,” he added. “There’s just no way. The last I saw, we had 77% of staff vaccinated with two shots.”
The key, he noted, were exemptions, which he pegged at about 15% to 20% of the workforce, based on anecdotal evidence.
“That’s what we’re seeing from talking to some of the bigger companies, and I think that will be pretty much consistent across the board. The majority are religious and about 5% or so will be medical. As long as exemptions are in place, we should be OK. That doesn’t mean we aren’t still looking for staff, though.”
He said that his members “figured out” their policies and procedures “about 60 days ago,” which would have been just after the U.S. Supreme Court allowed CMS’s healthcare worker mandate to proceed. Members have kept their religious exemptions “fairly tight,” Voepel added, noting some applications for them have been denied.
Exemption policies will be pivotal in many locations’ quest for vaccination compliance. In Arizona, for example, the state health department first will cross-reference a facility’s vaccination and exemption numbers against what was reported to the Centers for Disease Control and Prevention national database. Then surveyors will randomly pick a small percentage of on-site exemption documents to verify them, Voepel said he was told.
“It doesn’t sound like they want to get too far into it, but what’s ‘ridiculous’ in a bureau chief’s mind and ‘ridiculous’ in a surveyor’s mind can be two different things. We may see some issues down the road,” he cautioned, raising the ever-present concern of subjective survey findings.
Resources offered
A LeadingAge spokeswoman told McKnight’s that although the organization has heard concerns that the mandate can be a source of additional pressure for employers with recruitment and retention challenges, it hasn’t received any reports of significant employee exits from its provider members.
However, those who are struggling can take advantage of educational resources in order to boost vaccination and booster rates among staff, including its new education campaign, “CARE FULLY,” which focuses on vaccine hesitancy among minority workers.
“Our goal with this work was to develop a campaign grounded in respect and authenticity, so care professionals can reach a decision about vaccines and boosters on their terms,” said Susan Donley, senior vice president at LeadingAge, on Tuesday.





