
A newly-developed heat map of coronavirus cases in U.S. nursing homes and assisted living facilities will help to prioritize much-needed personal protective equipment and testing supplies for hard-hit providers.
Its creation was announced the same day a major provider group delivered scolding thanks about a plan for emergency responders to start sending personal protective equipment to providers the first week of May.
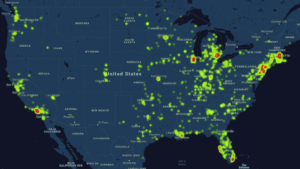
The map was launched as a collaborative effort between the Society for Post-Acute and Long-Term Care Medicine (AMDA) and pharmacist association ASCP. The organizations used publicly available data released by at least 23 states to develop the map, which displays the presence of COVID-19 in facilities at a ZIP code level.
“When we launched this, we knew that it wouldn’t be a complete picture but it would be a good start,” AMDA Executive Director Christopher Laxton, CAE, told McKnight’s Long-Term Care News. “We need to shine a light on areas that are hotspots, and the heat map shows those.”
The map illustrates that facilities in southern Florida, New York, New Hampshire, southern California, Chicago, Minneapolis and Seattle areas are among the hardest hit.
“Those are the folks that really need to be prioritized for access to PPE, access to testing, additional bed capacity, additional staffing, basically all the things that are currently preventing us from containing the spread within our very vulnerable nursing home population,” Laxton added.
Providers will also soon be required to report their coronavirus data directly to the Centers for Disease Control and Prevention once guidance and a reporting mechanism is released by the federal government.
Laxton said the CDC is working with provider groups to put together its reporting tool, which he said still “may be a couple weeks off.”
“Once that data becomes available and public, we’re going to overlay that onto the heat map, so we’ll have a more complete picture,” Laxton said. “That’ll be very useful.”
He added that the map serves as a “straightforward national picture of nursing home COVID prevalence” and encouraged providers to continue to share their data.
“Even though we see the curve flattening in the general population, it’s not flattening in nursing homes. It’s really important for us to be able to show immediately this is where we need some attention and aid,” Laxton said.
FEMA to alleviate ‘disgraceful’ PPE situation
Reports that the Federal Emergency Management Association will be distributing PPE to nursing homes starting in early May depict a long overdue move by the federal government, LeadingAge officials said Tuesday. Gear reportedly would be sent in stages for about five weeks, sending each nursing home weeks’ worth of supplies.
CMS Administrator Seema Verma alluded to the pending development in an April 20 press conference, while both ABC and NBC news reports subsequently have added details.

“This is the first sign in months that our calls for personal protective equipment (PPE) prioritization for providers of aging services are being heard,” LeadingAge President and CEO Katie Smith Sloan said in a statement.
“It is disgraceful that PPE and testing were not prioritized for older adults in the early days of this pandemic, even though it was widely understood from the outset that older adults and caregivers were at the greatest risk,” she added.
The organization added that PPE is one of the only tools providers have to combat the pandemic. Despite not receiving enough PPE or testing, healthcare workers have still shown up everyday to care for residents, potentially putting themselves and their families at risk.
“The only way to avert this slow-motion catastrophe is to provide meaningful levels of PPE, as well as effective and efficient testing and a comprehensive approach to supporting older adults and the workers who care for them,” Smith Sloan said.





