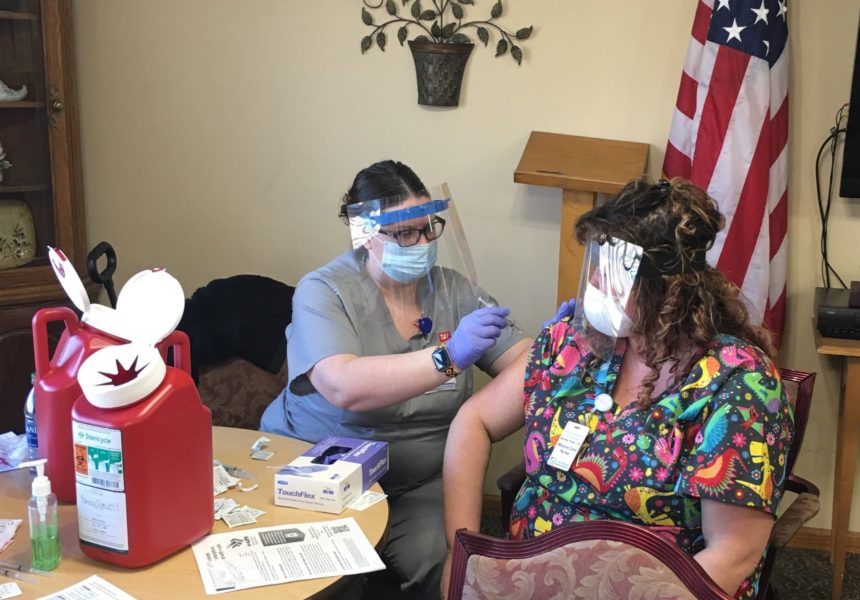
Providers say they are onboard with a new COVID-19 vaccination reporting mandate announced by federal health officials on Tuesday — calling the additional transparency “critical” for the industry to meet its own staff vaccination goals.
“Vaccines are the most important development of the pandemic for older adults, and LeadingAge encourages all staff and residents to get vaccinated — and for providers to report. But to meet CMS’ goal of increased vaccination rates, more must be done,” acknowledged Katie Smith Sloan, LeadingAge president and CEO, on Tuesday.
New mandate
The Centers for Medicare & Medicaid Services early Tuesday announced an interim final rule requiring long-term care and intermediate care facilities to report weekly COVID-19 vaccination data for both residents and staff.
Enforcement of the rule will begin June 14. Civil monetary penalties may be imposed for failing to report COVID-19 vaccination rates, similar to actions that may be taken concerning rules for flu and pneumococcal vaccines, officials said.
Facility-specific vaccination levels will be posted publicly on the agency’s COVID-19 Nursing Home Data website as more information becomes available, according to CMS.
LTC facilities are currently required to report only COVID-19 testing, case and mortality data to the National Healthcare Safety Network for residents and staff — but not vaccination rates.
The new rule is designed to assist in monitoring uptake among residents and staff, and aid in identifying facilities that may be in need of additional resources to respond to the COVID-19 pandemic.
Current official vaccination data for long-term care facilities nationwide was not clear at production deadline. But CMS previously said that approximately 22% of LTC residents and 62% of staff initially declined the vaccine during the federal sponsored vaccination clinics.
The agency added that “provisional CDC data suggest that uptake increased over time as the safety and effectiveness of the vaccines has become better understood, and approaches that ameliorate vaccine hesitancy have been identified.”
“Without a reporting requirement, we will have no way to identify those nursing homes with low vaccination rates so that they can be supported by educational outreach and their residents and staff protected by vaccination,” CMS wrote.
More transparency
Industry stakeholders, who have set a 75% staff COVID vaccination rate goal by the end of June, said the move will help them reach that target.
“We have been supportive of publicly reporting COVID-19 vaccination rates in long-term care since the vaccines were first approved, and we greatly appreciate CMS taking this step [Tuesday],” said David Gifford, M.D., chief medical officer of the American Health Care Association. He also stressed that transparency on vaccination rates should be expanded to all Medicare providers.
“Reporting vaccination rates is critical to facilitating in-person visitations in nursing homes, tracking the effectiveness of the vaccines, and helping ensure the industry meets our goal,” he added.
Gifford and Sloan both cautioned that nursing homes have many of the same struggles as the general population in getting certain groups vaccinated.
“It is important that we not judge facilities with low vaccination rates, but instead, seek to understand whether additional resources or outreach can be done to encourage more staff and residents to get the vaccine, or help facilities acquire additional vaccines for new patients and hires,” Gifford said.
Sloan added, “There are varied and valid reasons — that are out of providers’ control — why residents, families and staff may not yet feel comfortable with vaccines.
“As with so much of the pandemic, this is a community issue that requires a community response,” she continued. “Continued education about and support for vaccines must come from many different voices to achieve success.”





