
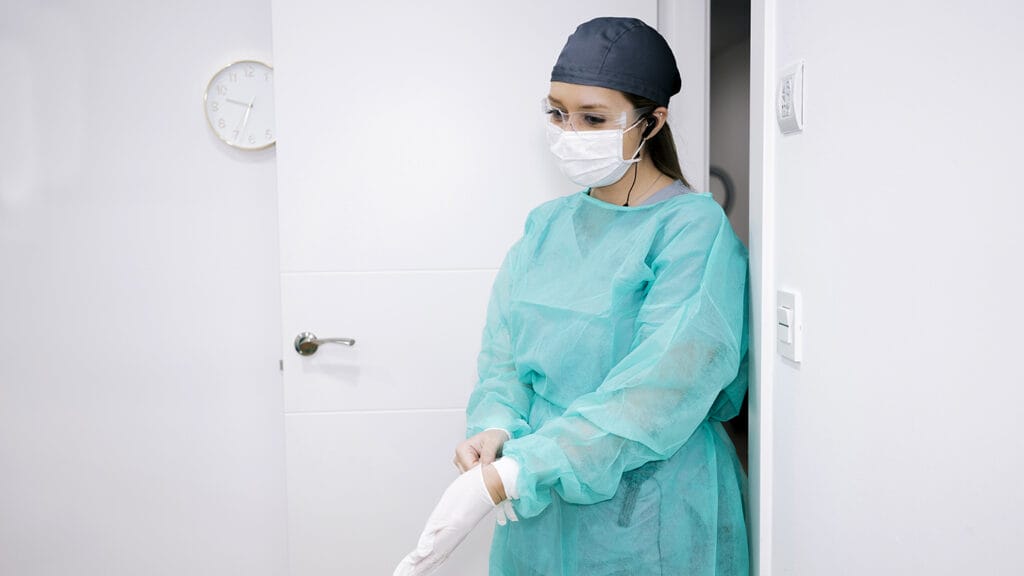
A new set of regulations requiring the use of enhanced barrier precautions for many nursing home patients has left providers scrambling to understand the rationale behind some standards and grappling with the potential costs, according to callers on a Tuesday Open Door Forum.
Providers from several facilities pressed officials from the Centers for Medicare & Medicaid Services about how to interpret the new rules — especially since surveyor guidance for the regulations hasn’t yet been published.
The use of the extra precautions for patients carrying or infected with multidrug-resistant organisms, or MDROs, and those with chronic wounds or indwelling devices went into effect Monday.
CMS officials described the adoption of the gown-and-glove guidance established by the Centers for Disease Control and Prevention as an effort to “align with nationally accepted standards.”
But nursing home representatives on the hour-long call inundated those officials with concerns about possible discrepancies and how to interpret some of the rules’ intricacies and flexibilities.
A caller who had met Tuesday with a state organization on the enhanced rules questioned why they allow for non-gowned and gloved transfers of patients in some common areas, such as dining rooms, but not in others, such as a therapy gym. She called the different standards “counterintuitive.”
Time and money the big concerns
Christine Teague with the CMS Division of Nursing Homes told the woman that the difference comes down to how much time the interaction might take. Therapists in close, prolonged contact with an infected patient or those with other risk factors need to be gowned and gloved during every interaction. So, too, does anyone working with a patient on the EBP protocol in their room and delivering personal care.
That requirement, in particular, is raising concerns among many nursing home teams.
“Has anybody done any kind of study to see what the increased cost is going to be for gowns and gloves because of this, and how it is going to affect the psyche of our residents that we are now going to be having to wear gowns and gloves all the time in the rooms?” asked the same caller, identified only by her first name.
“We are merely embedding CDC’s recommendations into our guidance so if there are questions like that, I would encourage you to reach out to the CDC,” responded Evan Shulman, director of the Nursing Home Division.
Still, others raised similar concerns throughout. Multiple callers from pediatric long-term care facilities noted that nearly all of their patients would need to be placed on EBP protocols because almost all of them have G-tubes, a type of indwelling device that triggers the new requirements.
“This guidance would then extend to almost 100% of our residents, and I’m just wondering the
considerations for that, given the anticipated negative impact on their emotional and psychological development,” another caller said. He noted that the inclusion of feeding tubes in the CMS guidance appeared to be a departure from the CDC standard that applies only to individuals who are identified as having certain MDROs.
“That requirement doesn’t extend to patients with indwelling catheters, which is basically a requirement to be in a pediatric long-term care facility,” that caller added. “So now in effect, 100% of our patients would now apply to this measure, not just individual patients within a unit.”
CMS: Determine on the go
Others questioned how and when they should determine whether to use EBPs, and Teague said those evaluations should be done on an “ongoing basis.”
“That would be whenever the resident is admitted; whenever they go out to the hospital, they are readmitted and returned to the facility; if they have a change in condition; if they have a new
wound that may change their status as far as needing to use EBP; a change in the indwelling catheter or indwelling medical device,” she said. “All of those things would necessitate the facility to reevaluate the resident to determine whether or not EBP are appropriate.”
Others wanted to know more about the possibility of reusing washable gowns for the same patient and by the same staff member, as well as where to store gowns so that they could be easily accessible to staff entering patient rooms.
While the regulations require EBPs for residents with organisms targeted by the CDC, the new CMS regulations leave facilities to decide how they will approach patients with other, “epidemiologically important” MDROs, such as MRSA. One caller noted that CDC websites provided as resources by CMS give nursing home staff “no real way to discern” when to incorporate the use of additional personal protective equipment.
Despite any lingering questions about the regulations — which went into effect only about 10 days after being issued — Shulman said providers should be in compliance immediately.
“There is no grace period,” he said. “We know that the enhanced precautions have been out for quite some time from the CDC. … We also find in our guidance that we try to give facilities as much flexibility as possible to be creative in how to identify residents that require precautions. … We will continue to evaluate it as it progresses, but there is nothing stated in our guidance about any grace period, and we think that providers should be able to adopt this.”




