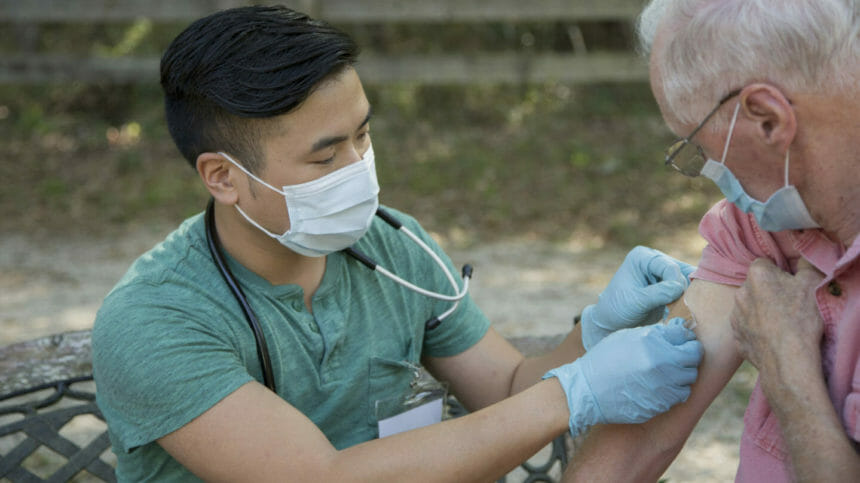
COVID-19 vaccinations are well underway in long-term care, and facility cases are on a downward trend, but the need for stepped-up infection control measures likely will remain a necessity for the foreseeable future, say industry observers and stakeholders.
One key unknown is how Centers for Medicare & Medicaid Services guidance on testing and other mitigation efforts will change if case counts continue to fall.
“We are all waiting on CMS to update their policy on a number of areas, including staff and resident testing, activities allowed within facilities, and family visitation, as more and more nursing home residents are fully vaccinated,” geriatrician Kathleen Unroe, M.D., MHA, told the McKnight’s Clinical Daily.
Because testing protocol is tied to county positivity rates, facilities certainly will see an effect as those infection numbers go down, said Unroe, a long-term care researcher and professor from Regenstrief Institute and Indiana University School of Medicine. “But the substantial impact will only happen if policies change to reflect the role of vaccinations,” she added.
There is also the matter of how many people will get vaccinated and when, said Chuck Cooper, global vice president, medical and scientific affairs, integrated diagnostic solutions and global health, Becton Dickinson & Co., or BD.
“There’s a lot of optimism, and rightly so,” said Cooper, whose company supplies point-of-care rapid COVID-19 tests to long-term care. At the same time, vaccination levels may take some time to make a big enough difference in U.S. infection rates to support infection protocol changes at the facility level, he said. “We need to have a certain percentage of the population with some level of protective immunity that’s been vaccinated.”
What’s more, it’s uncertain how long immunity from approved vaccines will last and how new virus variants might affect that protection and virus transmission, Cooper added. “We don’t even know yet whether or not there is a seasonality to this virus … similar to what we see in other respiratory viruses,” he said.
And the thorny reality that not all individuals are willing to get vaccinated may play a part in continued spread, according to Krutika Kuppalli, M.D., assistant professor of infectious diseases at the Medical University of South Carolina. In addition, “no vaccine is one hundred percent effective, so there will be some individuals who still develop COVID-19 and we will need to be able to detect those cases,” she told McKnight’s.
Federal health officials, meanwhile, are said to be discussing new mitigation guidance for people who are fully vaccinated. The Centers for Disease Control and Prevention last week relaxed its quarantine recommendations for those patients. But the agency was very clear that the new guidance shouldn’t apply to healthcare workers and residents in facility settings, except perhaps to help mitigate staff shortages when there is no other solution.
There are also no changes yet to the agency’s post-vaccination infection control protocol for long-term care residents, most recently updated in December. All symptomatic residents should continue to be assessed and cases handled as though the resident is infected with SARS-CoV-2 virus until they’ve been cleared — even if they’ve been vaccinated, it advises.
No more isolation
BD’s Cooper is optimistic about the possibility of expanded community testing to further reduce asymptomatic transmission, which could add to the impact of vaccinations in reducing staff and resident infections. But the most vulnerable must be protected while these possibilities are explored, he said.
“What we have learned is that respiratory viruses like influenza and SARS are survivors,” test maker Quidel Corporation added in response to a query. “They mutate regularly and eventually variants will emerge that are not neutralized by the antibodies generated from existing vaccines. …So, at least for the next few years, as we globally immunize or we develop new vaccines for the [COVID-19] variants, our other lines of defense — masking and social distancing and frequent testing — are still going to be required.”
But geriatrician Unroe is adamant that isolating residents is one measure that can’t continue as currently practiced. She foresees long-term care adapting to its new infection control realities in a way that makes more sense for residents.
“Re-opening to visitation, re-connecting families with nursing home residents, is critical,” she told McKnight’s. “I am confident we are capable of doing so safely; keeping people apart continues to impact [their] health and well-being.”




