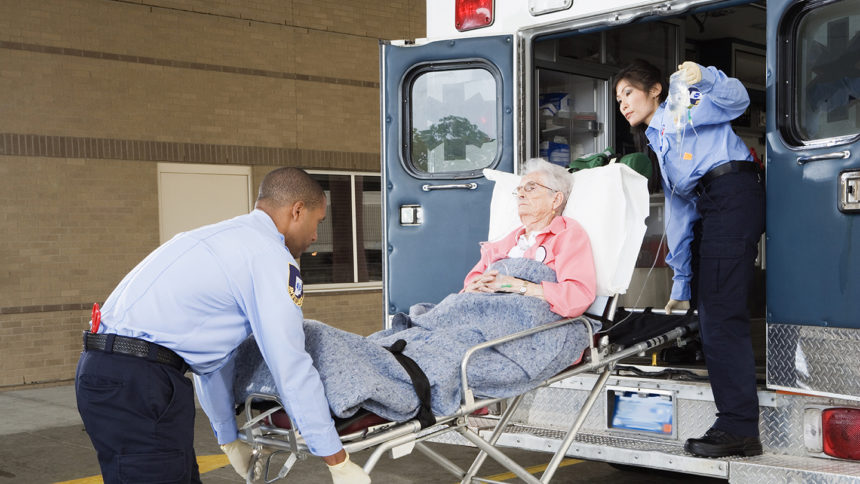
Nursing homes in Washington state may get a reprieve from a labor crisis that is stranding potential residents in hospitals.
Unable to attract enough workers to meet staffing minimums, many nursing homes across the US have closed wings or units or restricted new admissions over the past year. That means hospitals have far fewer options when it comes time to refer patients for post-acute care.
Companion bills introduced in the Washington Senate and House introduced late last month would update Medicaid funding rates for skilled nursing facilities every year instead of every two years as is the current system and create an inflation adjustment to better estimate the cost of care. The two bills each have a Democrat and Republican lead sponsor, marking comity between two parties that are normally at odds with each other, underscoring how critical these staffing issues have become.
Although the state’s skilled nursing facilities have been struggling against a labor shortage for some time now, the worsening hospital logjams led the Washington State Hospital Association to make increased post-acute care funding a legislative priority in 2023.
“This legislation will help ensure vulnerable populations that are on Medicaid have a place to stay for treatment and rehabilitation,” Sen. Kevin Van De Wege (D-24th District) said in a statement provided to McKnights Long Term Care News.
Hospitals backups have become a hot-button issue for health systems and politicians. Facilities in states as disparate as New Hampshire and Nebraska reported extensive wait lists, understaffed nursing homes threaten to block up the entire care continuum.
The American Health Care Association detailed some of the worst stories last fall, and by some accounts, the crisis is only escalating.
In Washington, nursing homes were underpaid by $620 million over the last five years, according to information from the Department of Social and Health Services, which, combined with pandemic-related labor shortages have resulted in understaffed facilities that are closing units or wings or halting admissions.
“The safety net for our low-income elderly is seriously strained by Medicaid funding policies that have failed to keep up with Washington’s operating costs required for care, including labor, food, nursing supplies, equipment, and utilities,” Carma Matti-Jackson, CEO of the Washington Health Care Association, said in a statement provided to McKnights. “The failure to adequately fund rates translates directly to the bedside. When providers cannot compete for workers because of inadequate funding, the disruptions are significant both to seniors needing long term care and to the remaining workers delivering those services. There is a great human cost to patients, families, and caregivers.”
The association was sounding alarms about the staffing crisis as far back as July 2021, when it sent a letter to Gov. Jay Inslee (D) saying the pandemic “exacerbated an existing crisis” that was threatening the care of 100,000 nursing home residents across the state, according to a report from King5 news.




