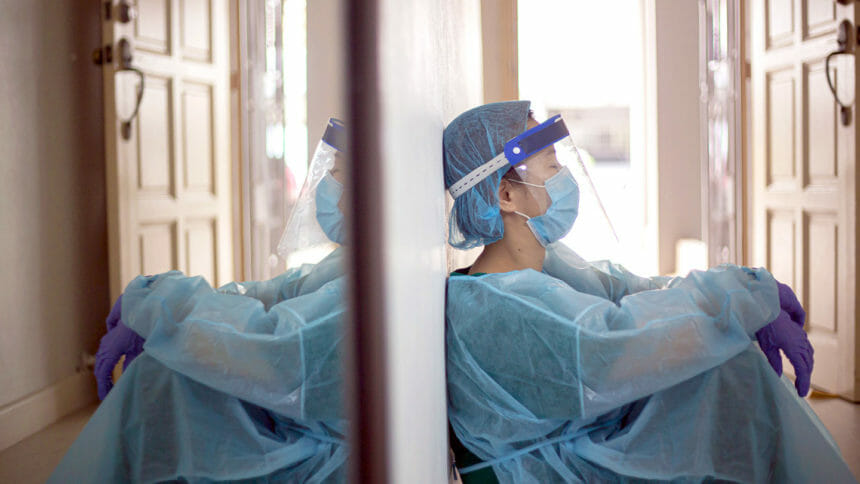
The national response to the pandemic failed to protect residents — and their caregivers — emphasized a prominent healthcare policy researcher Monday after the New York Times published an article that some might have wrongly interpreted as holding nursing homes solely responsible for high COVID-19 death and infection rates.
David Grabowski, a researcher at Harvard Medical School, was one of several experts interviewed for the article “How Nursing Homes Failed to Protect Residents From Covid.” Grabowski co-authored a study on the lack of antivirals’ uses in nursing homes that was cited in the article.
He told McKnight’s Long-Term Care News on Monday that nursing homes were not blameless, but that the bigger fault lies with policymakers. In the Times article, Grabowski and study co-author Brian McGarry, both gave the health care system a “D” grade overall for nursing homes’ pandemic outcomes and performance.
“I was not assigning that grade to nursing homes or their staff,” Grabowski clarified in an email to McKnight’s. “I assigned a D grade to our overall policy response in protecting nursing home residents and their caregivers. I would include policymakers at all levels (federal and state). They were slow to get facilities personal protective equipment and rapid testing. They kept families out of nursing homes for far too long. They are now slow in getting antivirals to these residents.”
The research from Grabowski, McGarry, and others found that just 18% of COVID cases in nursing homes were treated with antivirals and that 40% of facilities reported not using antivirals at all. The research, Treatment of SARS-CoV-2 Infection in US Nursing Homes, 2021-2022, was published last month in JAMA. During the study period, there were 763,340 cases of COVID among nursing home residents, but only 136,066 residents — or 17.8% — were treated with antivirals.
At least 167,000 patients and 3,100 nursing home workers have died due to Covid-related conditions, according to federal statistics.
The article noted that nursing homes were shorted on protective equipment since the federal government prioritized hospitals over other healthcare facilities. COVID-19 test kits that were eventually sent to nursing homes were underutilized since it took too long to get results back from a lab to make them worthwhile for screening employees, it added.
The NYT report also was critical of the lockdowns, which “continued for far too long,” and of efforts to push more nursing home staff to get vaccine boosters.
“I am not letting nursing homes off the hook,” Grabowski explained in his email to McKnight’s. “Many did the best they could under trying conditions, but some did not. We should hold those facilities accountable. However, when I think about the crisis in nursing homes during the pandemic, it was largely a system failure rather than a crisis caused by a few bad apples.”



