
Lawmakers must take a “clear stance” to address gray areas in discriminatory tactics being used by some nursing homes to reject less profitable residents, stressed an industry expert Tuesday.
“We actually need lawmakers and regulators to do more to help codify and build on those rights,” said Ashvin Gandhi, health economist and assistant professor at UCLA said during a webinar hosted by the Long Term Care Community Coalition, where he presented his latest findings on admissions discrimination in nursing homes.
Using California nursing home resident data from 2004 to 2007, Gandhi analyzed patterns by using this test: Do the same facilities admit different patients depending on how full they are?
“The short answer is yes. Yes they do,” he emphasized.
He compared the characteristics of residents who are admitted to facilities on their least full days versus those who are admitted when facilities have more open beds available.
He said that on average, as facilities become more full and it becomes more costly to admit less-profitable patients, “suddenly you see them admitting fewer long-stay residents, avoiding Medicaid patients and residents who have visual impairments.”
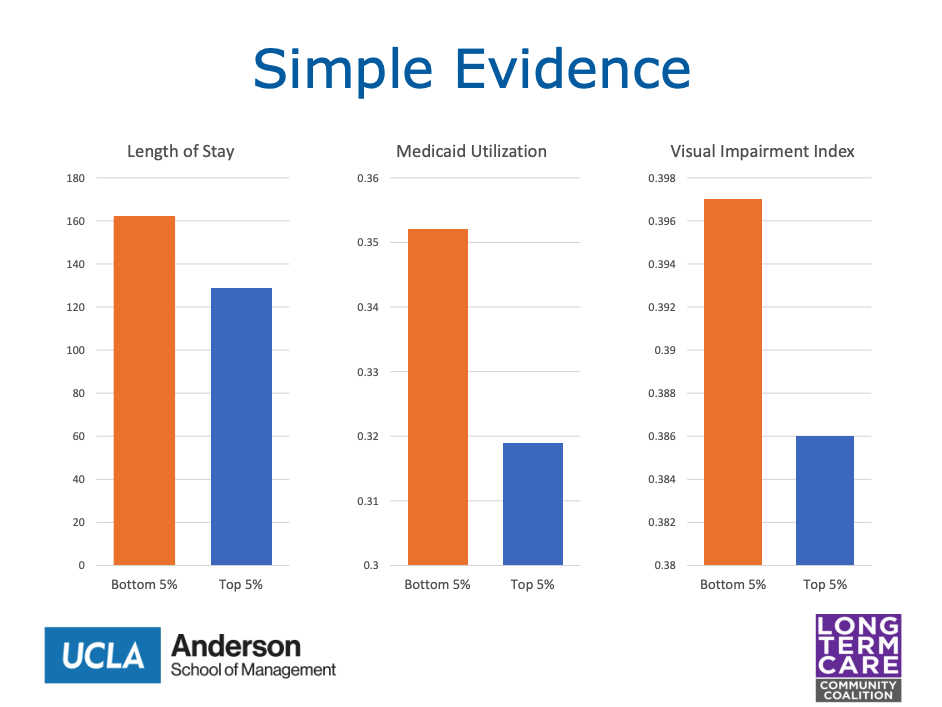
“This evidence is really consistent with facilities adjusting how discriminatory they are based on how full they are,” he said.
Using machine learning techniques, he also put to test which types of residents are typically admitted on lighter occupancy days. He found that long-stay and Medicaid residents were more likely to be discriminated against.
He also discovered that about 20% of Medicaid residents were not at their first choice facility. That figure was even higher (49%) for long-stay Medicaid patients.
Gandhi explained that existing law shows that disability discrimination is “clearly illegal” through the Rehabilitation Act, American with Disabilities Act and Fair Housing Act. That’s less clear when it comes to using Medicaid as a form of admissions discrimination, he added.
He said the 1987 Nursing Home Reform Act has a “clear intention to ban it” by prohibiting providers from asking residents to waive their Medicare or Medicaid rights. However, there are potential loopholes where facilities can deny admissions without asking residents to forgo Medicaid.
“They’ll simply look at the resident, ask for their financial status and then deny admission based on the fact that they’re on Medicaid or going to be on Medicaid,” he said. “It’s a clear violation of the intention of the law but some facilities would argue that it possibly satisfies the letter of the law.”
This is an area where there’s a clear role for advocates and lawmakers must step in, he said.
“Regulators must take a clear stance on the law or it will stay a gray area,” Gandhi said.
Policy solutions he suggested included having facilities admit residents on a first-come, first-served basis and raising Medicaid reimbursement rates. But the best solution, he said, would be to invest in expanding the capacity at high-quality facilities.
“Admissions discrimination in nursing homes is really, really widespread,” he said. “Being able to go to a facility that has better staffing, higher quality — even if you set COVID aside — has really really dramatic implications for the health and welfare of these older Americans.”
Providers in the past have faced many accusations for denying admissions for patients they believe they can’t care for, particularly in regards to residents with opioid use disorder. The American Health Care Association last month said that long-term care facilities must adhere to government requirements, and that the federal government specifically prohibits nursing homes from accepting patients for whom they cannot provide appropriate care.





