
“Exceptional SNF” is an actual skilled nursing facility based in Cleveland. Though its name isn’t really Exceptional, so much of what it does really is.
Exceptional SNF developed a center of excellence around cardiac rehabilitation. It became a magnet facility by partnering with a prominent cardiology physician group and by adopting the care protocols of its referring hospitals.
Exceptional SNF utilized appropriate structure, process and outcome measures. Despite this, however, it might have better been called “Mediocre SNF.” Though it achieved its structure and process key performance indicators (KPIs), it was not exceptional when it came to outcomes.
Its observed rehospitalization rate was higher than local benchmarks, and while many patients who entered their program succeeded, a large proportion did not.
Have you ever wondered why some patients or residents, with the same diagnoses as others, have unplanned transitions to hospital while others do not?
In our fast-paced world and lack of access to timely information, it’s not always easy to find patterns or trends in your own (re)hospitalization data. However, this was not the case for Exceptional SNF. It had fully committed to using its data and analytics for QAPI and marketing/census development. Here is what its leaders learned.
Most patients who returned to hospital within 30 days after being admitted to its cardiac rehabilitation program had moderate-to-high cognitive impairment (CI). In fact, when you factored out this cohort (removed them from your sample), its rehospitalization rates were well below average and the average length of stay went up by three days.
Wouldn’t life be grand if every solution to life’s challenges were to remove them from your sample? But alas, it is not that simple. Yet, knowing that the presence of CI did have a significant impact on this SNF’s rehospitalization outcomes is an even more meaningful insight.
I suspect you’ve had similar insights along the way and, like me, believe that dementia or other comorbidities can impact the success of a patient’s post-acute stay. This was the motivation for this study we conducted.
We looked at patients who were admitted to over 3,000 SNFs between 2015 and 2017. We defined CI as a Brief Interview for Mental Status (BIMS) < 13 or Cognitive Performance Scale (CPS) > 2, or I4800 (Non-Alzheimer’s Dementia) or I4200 (Alzheimer’s) checked on the Minimum Data Set (MDS) 3.0.
If you’re not a connoisseur of the MDS, simply stated: We identified patients with cognitive impairment either by a cognitive assessment scale or formal diagnosis. If you are a connoisseur, thank you!
Here is what we found when we compared the observed rate of rehospitalization, measured by PointRight® Pro 30® for those patients with CI and those without:
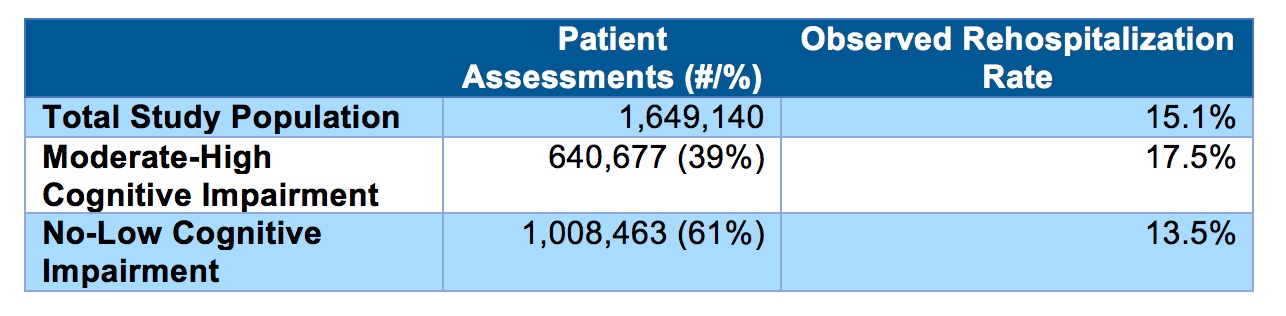
The four-percentage point difference is not only statistically significant, but from a clinical and business perspective, it is also guiding.
A study in the Gerontologist titled “Transitions From Hospitals to Skilled Nursing Facilities for Persons with Dementia: A Challenging Convergence of Patient and System-Level Needs” supports this finding. SNF nurses identified “inaccurate/limited hospital discharge communication regarding behavioral symptoms, short discharge timeframes and limited nursing control over SNF admission decisions” as contributing to poorer patient outcomes, including rehospitalization.
Seldom is information around CI, behaviors, depression, skin conditions, pain and other challenging comorbidities accurately and consistently communicated during care transitions. However, what is always communicated: expected length of stay!
The next finding I’m about to share admittedly caught me off guard. We approached this study with the hypothesis that CI would increase rehospitalization AND hospitalization, assuming comorbidity would mask or otherwise complicate the presentation of symptoms that if treated would avoid hospitalization. Remember that hospitalization is not the “return” to hospital, but the hospitalization of the long-stay resident.
We measured hospitalization using PointRight® Pro Long Stay™ observed rates, which includes in its denominator those residents who have been in the SNF for 100 or more days.
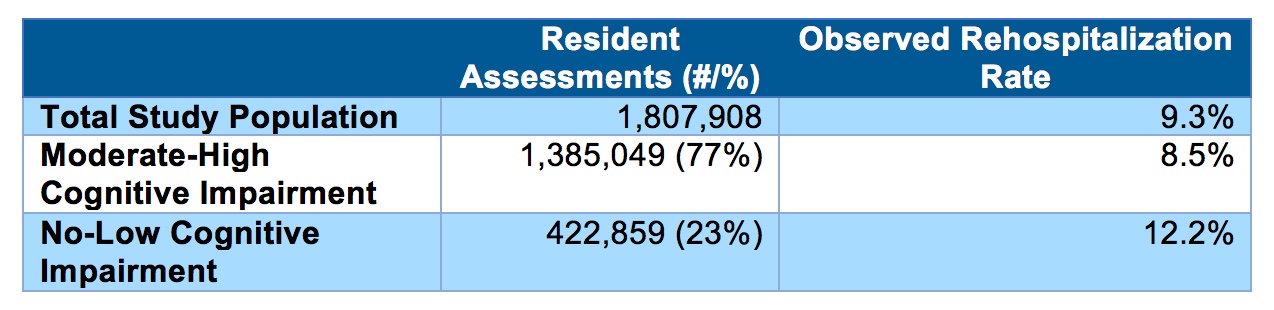
Do these findings surprise you? Seventy-seven percent of the long-stay population had CI; the low rate of hospitalization suggests that we better understand this population within our long-stay environment.
How did this information help Exceptional SNF?
1. Its best practices, particularly those adopted from the acute space, took into consideration these pertinent comorbidities, such as cognitive impairment. They incorporated more geriatric-specific practice guidelines, for organizations such as AMDA.
2. They now share insights from root-cause analysis with referring sources. This compelled them to include information about CI at time of discharge.
3. When dialoguing around expected LOS, they communicate the impact of CI on this outcome (add three days!).
4. They took lessons from “the other side of the house.” They realized that the interdisciplinary team caring for their long-stay residents may have some terrific insights into the needs of their post-acute population with CI.
One final comment: We own this. This is not a tale of woe about the hospital system that didn’t communicate. It is for us, dedicated SNF/long-term care/nursing home professionals, to accurately identify and manage these comorbidities that are inherent in the geriatric population.
Seminal research published in The New England Journal of Medicine stated, “Dementia is a leading cause of death in the United States but is underrecognized as a terminal illness.”
Clinical leaders understand this better in our long-stay population than short-stay.
Steven Littlehale is a gerontological clinical nurse specialist, and executive vice president and chief clinical officer at PointRight Inc.





