
I recently had the pleasure of hearing a COO of a group of nursing homes present a closing session at their organization’s annual meeting.
The company’s nursing teams, administrators and MDS Coordinators had spent a week together learning of regulatory updates, sharing ideas, and determining best approaches to practice in the coming year.
His presentation, however, tasked them with taking all this knowledge to then determine if they were truly meeting the needs of those they serve daily.
He used Maslow’s theory as a guide and challenged the group to aim for promoting care that allows for a level of esteem in person centered care.
To provide some background on how these needs are defined, Maslow (1943, 1954) stated that people are motivated to achieve certain needs and that some needs take precedence over others.
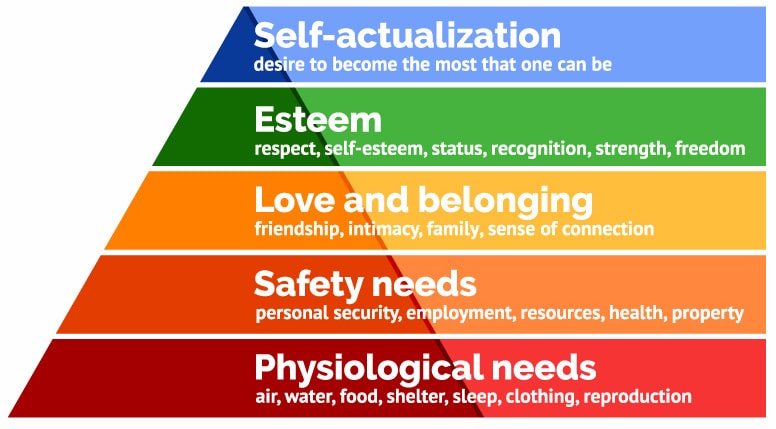
As care providers, the first two levels, physiological and safety, are standards of care. We assist in meeting the basic need is for physical survival, and we keep individuals safe.
Moving up the tiers, however, requires us to have a greater level of understanding and knowledge of individuals residing in our communities.
Sound familiar to shifts we are seeing from the Centers for Medicare & Medicaid Services?
Those of us who have attended (either live or virtually) the two days of CMS QRP training this week, are aware that regulatory changes are paving the way for use to have greater granularity and understanding associated with clinical care needs.
The next tier is associated with love needs, which can be met only after physiological and safety needs have been fulfilled. This tier also involves feelings of “belongingness.” Examples include friendship, trust and acceptance.
Esteem needs are defined in the next tier and include elements associated with independence and respect from others.
The most obvious alignment in SNF care with esteem is that we allow individuals the opportunity to perform tasks as independently as possible, and in short, that we do not create excessive levels of dependence or impairment by providing excessive levels of care.
Remember: This is also clearly outlined in how we are instructed to score Section GG functional status for self-care and mobility. I like to think Maslow would be proud of this requirement.
Residents should be allowed to perform activities as independently as possible, as long as theyare safe.
You meet safety needs first and then you can move on to esteem and independence.
Further opportunity to achieve the esteem level as a caregiver requires you to have a complete understanding of specific interests and motivators for your patients.
I will use myself as an example, in the hope that if I end up in long-term care, someone will understand my motivations.
You may see me as an elder cueing others to throat clear and re-swallow in the dining room … or attempting spaced retrieval with someone who can’t seem to remember her room number or where to find the activities calendar.
What I really hope is that by that time, esteem needs are not attempting to be met with an activities calendar but that motivating tasks are simply ingrained into the natural scheme of the day.
For me, if this speech therapy gig doesn’t work out, I would make one heck of a Molly Maid. Seriously.
People who know me professionally know that I love the process of creating, teaching and implementing new processes in the post-acute care industry. Nothing is more gratifying than seeing an idea big or small become a reality and then measuring its impact on clinical care.
Well, maybe there is one thing as gratifying … For me, it is the smell of a house freshly cleaned with Murphy’s Oil and Clorox. Add some ammonia on top, and life is good.
A clean house helps me to have a sense of esteem.
Made beds are proven to result in me having a more productive work day.
With that said, back to work for me!
MDS training updates, clinical pathway finalization and spreading more QRP goodness.
Right after, of course, wiping down this desk …
Renee Kinder, MS, CCC-SLP, RAC-CT, is Vice President of Clinical Services for Encore Rehabilitation and is the Silver Award winner in the 2018 American Society of Business Publishing Editors competition for the Upper Midwest Region in the Service/How To Blogs category. Additionally, she serves as Gerontology Professional Development Manager for the American Speech Language Hearing Association’s (ASHA) gerontology special interest group, is a member of the University of Kentucky College of Medicine community faculty, and is an advisor to the American Medical Association’s Relative Value Update Committee (RUC) Health Care Professionals Advisory Committee (HCPAC).




