
Now that the much-anticipated October 1 implementation of MDS Section GG has come and gone, a number of questions regarding best practices for collaboration among skilled nursing interdisciplinary teams have emerged.
Common work among departments always can be tricky, and this instance is no exception.
On the positive side, however, the need for interdisciplinary partnerships has led to increased communication, collaboration and awareness related to the functional abilities and desired functional outcomes for the individuals we serve.
To refresh memories, the IMPACT Act of 2014 mandated the establishment of a SNF Quality Reporting Program. In order to effectively meet the requirements for quality measure reporting via a standard assessment tool, CMS responded by developing Section GG as a new section of the MDS for Medicare Part A patients.
Section GG includes self-care and mobility functional measures, some of which are derived from the CARE tool, as well as additional patient information and discharge goal reporting requirements.
Here are some key areas to keep in mind:
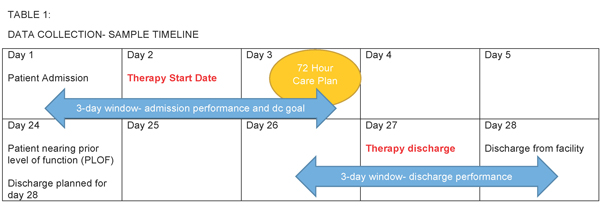
• Reduced time frame for data collection — The window for data collection is three days, which differs from the seven-day time frame we have for other areas of the MDS. Therefore, communication between Nursing and Rehab departments must occur early in the patient’s stay in order to set Admissions Performance and Goal Status areas for the Self-Care and Mobility sections.
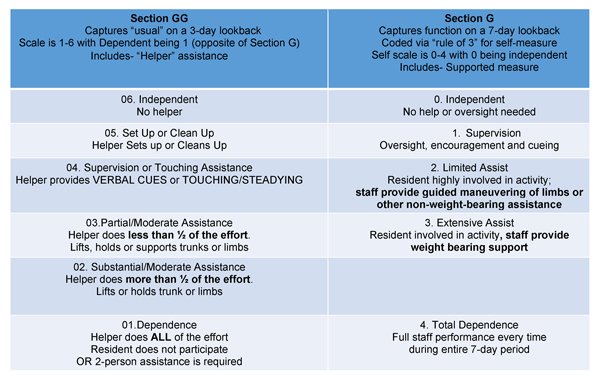
• New measurement scales — Remember that the Section GG scale is opposite of Section G and will likely differ significantly from the impairment level scales that rehab providers have within their internal electronic medical record systems for assessing baseline status and documenting prior level of function.
• Setting goal status — Plan of Care (also known as evaluation) documentation completed by the rehab teams will include essential elements that can assist the interdisciplinary team in setting goal status areas, including prior level of function for all rehab target areas.
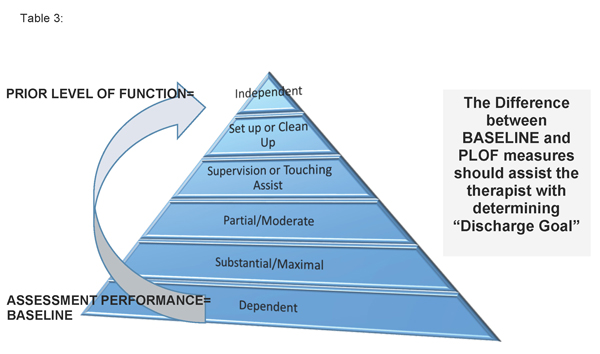
Additionally, remember that not all individuals will be able to return to full prior level of function, and the RAI manual does provide guidance on coding for individuals who will have goal areas that are the same as assessment performance and lower than assessment performance secondary to complexity or presence of a chronic, progressive, neurological condition.
• “Helper” assist — Helper assistance should be used only when a resident’s performance is unsafe or of poor quality, and providers should only consider facility staff when scoring according to the amount of assistance provided.
For the purposes of completing Section GG, a “helper” is defined as facility staff who are direct employees and facility-contracted employees (e.g., rehabilitation staff, nursing agency staff).
• Assistive devices — Activities may be completed with or without assistive devices. Use of any assistive devices to complete an activity should not affect coding of the activity.
FREQUENTLY ASKED QUESTIONS
1) With the implementation of Section GG, physical and occupational therapy should now complete assessments on all Medicare Part A patients in order to code. Correct?
Incorrect. The implementation of Section GG did not change the requirements for determining the need for skilled rehab care. In other words, “coding for Section GG” cannot be used alone as a reason for referral for therapy services. Additionally, all plan of care (POC) requirements per the Medicare Benefit Policy Manual remain intact and must be met for all rehab POCs.
2) OK, so rehab cannot evaluate for Section GG alone. Can rehab “screen” a patient in order to contribute to the coding at admission?
Screenings are “hands off” and no recommendations can be made from a screen alone, therefore screenings are not sufficient for Section GG.
3) Nursing says the patient needs a wheelchair and therapy says the patient is safe to ambulate. Should rehab complete a wheelchair assessment in order to contribute to wheelchair mobility coding?
Skilled rehab providers will be able to contribute only to portions of section GG for which they have assessed the patient. In instances where therapy does not see a skilled need to assess or treat various areas of the self-care and mobility subsets other interdisciplinary team members can collaborate to determine appropriate coding.
4) Does physical therapy complete all mobility and occupational therapy complete all self-care?
The discipline that completes the assessment specific to the coded area should be the discipline that contributes to the interdisciplinary team coding.
5) The nursing assistants “usual” differs from rehab “usual.” Is this a problem?
No. Remember that coding for section GG is an IDT process therefore variances are to be anticipated. Per the RAI: “[I]f there’s fluctuation in the performance of activities during the three-day assessment, the performance wouldn’t be the worst, and it wouldn’t be the best, but it would be what’s ‘usual’ for that individual.”
Renee Kinder, MS, CCC-SLP, RAC-CT currently serves as Director of Clinical Education for Encore Rehabilitation and acts as Editor of Perspectives on Gerontology, a publication of the American Speech Language Hearing Association (ASHA).





