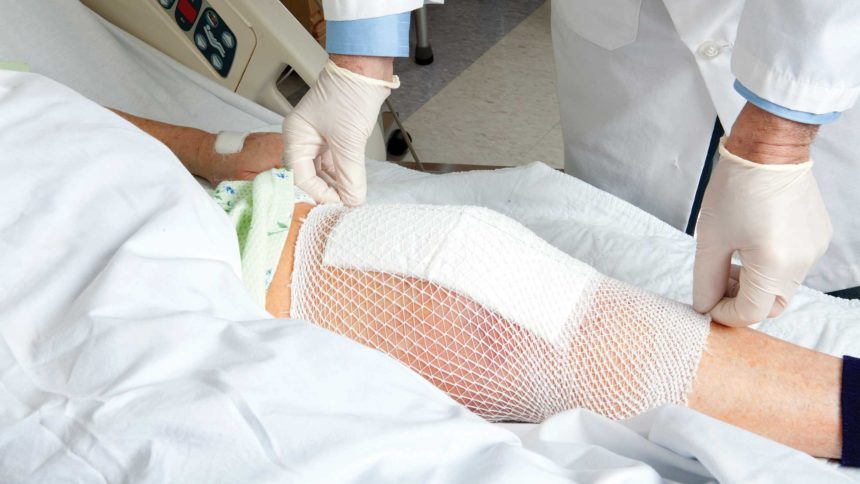
It’s well known that the coronavirus has inflicted immeasurable hurt on the elderly. According to data available at press time, while COVID-19 cases in all long-term care facilities accounted for 8% of total cases nationwide, they accounted for 41% of all COVID-19-related deaths, the American Health Care Association reported in October.
Perhaps symbolically, this impact has included the area of wound care, whose practices themselves have been touched negatively by the pandemic.
Reports have emerged that the virus may cause physiological changes that adversely affect the healing process. Experts also are beginning to echo concerns that providers’ pandemic response to the virus itself could be impeding wound care practice.
Complicating matters is the decision by many providers to ban or limit “nonessential” workers, something that some experts assert has hindered conventional wound care therapy.
“Residents with wound issues frequently have comorbid conditions that put them at higher risk for developing serious consequences from COVID-19,” said Karen Hoffmann, RN, MS, CIC, FSHEA, FAPIC, immediate past president of the Association for Professionals in Infection Control and Epidemiology.
Hoffmann explained that wound care among the elderly has suffered during the pandemic when routine medical visits, including many to wound clinics, were drastically reduced because this care was considered “nonessential.”
“Dressings may not have been changed as frequently as they should have been, or they may have been improperly changed, increasing the risk of infection,” she noted.
Others have voiced similar concerns.
“The hardest part of the pandemic is that it’s almost the exact same population that is most vulnerable to complications from COVID-19 that is most need of wound care,” wrote Brian Wallace, founder and president of Louisville-based NowSourcing, an infographic design agency, in a recent McKnights.com blog. “What’s been happening because of this is that caregivers have to make an extremely difficult choice. Do they take the risk of exposing their patients to the virus, or do they continue with the much-needed wound care?”
From the November 2020 Issue of McKnight's Long-Term Care News




