Despite reports of recent monthly gains in the number of long-term care employees, full recovery of the workforce could drag on until 2026 without substantive new assistance. That’s according to a report released Monday by the American Health Care Association and National Center for Assisted Living.
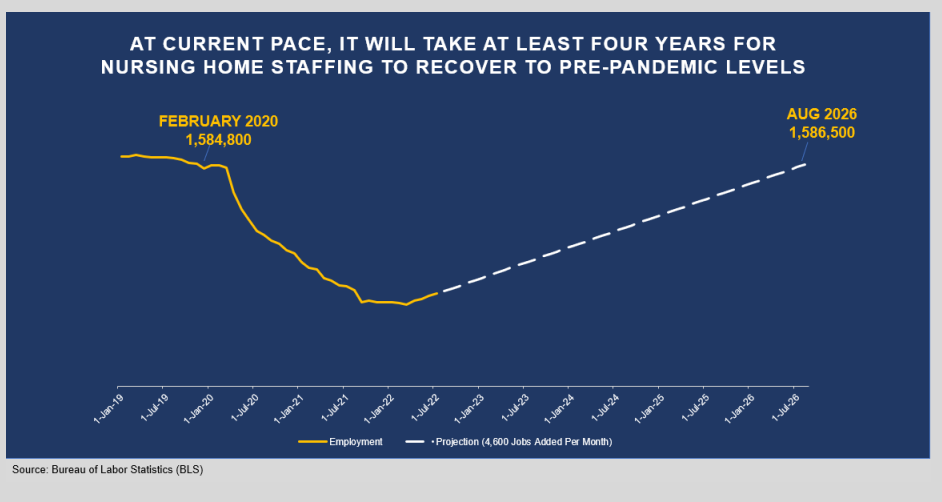
The industry has lost more than 362,000 employees during the pandemic, with 223,700 of those from nursing homes, the AHCA/NCAL report noted. Assuming little or no assistance is forthcoming, the group projects that the nursing home sector should grow by 4,600 jobs per month, based on average job gains from the last four years.
“Our caregivers, who are working themselves ragged, and our growing elderly population can’t afford to wait another four years,” said Mark Parkinson, president and CEO of AHCA/NCAL, in a prepared statement. “The long-term care workforce needs a boost now. We urge federal and state policymakers to put their support behind policies that attract and retain caregivers for our nation’s seniors.”
Bureau of Labor Statistics data from July 2022 shows nursing homes have seen the worst workforce losses of any U.S. healthcare sector since the beginning of the pandemic.
While the nursing home sector is still struggling with a workforce deficit of more than 14%, hospitals, physicians’ offices, outpatient care centers and other healthcare facilities have already reached or surpassed pre-pandemic staffing levels.
David Voepel, CEO of the Arizona Health Care Association, said the mandate for government involvement is clear.
Federal officials should prioritize long-term care with solutions such as student loan forgiveness, CNA to LPN to RN scholarships, and grants to both long-term care operators and universities to provide incentives to create formal partnerships and payment for tuition, he said.
“In Arizona, for instance, the state is helping long-term care on the SNF CNA/AL caregiver front by providing funding for the AHCA Works (Workforce, Outreach, Retention are the Keys to Success) program,” Voepel said. “This program helps recruit, pay for training and retention of CNAs and caregivers in Arizona facilities and assisted living communities.”
Staffing shortages have led 6 in 10 facilities to limit new admissions. The impact on access to care has a domino effect on other healthcare providers, especially hospitals that are unable to discharge patients when they need to free up space.
Voepel said he believes a disjointed educational system with a long-term network that is barely holding on is among the biggest impediments to restoring the COVID-ravaged nursing home workforce.
“In other words, nurse training is out there, but there aren’t enough proctors to handle the testing, and SNFs and AL communities don’t have the funding to hire the CNA/LPN/RN at a level to where they can afford to pay back their student loans,” he added. “We can start with a pathway for temporary nurse aids to become certified nurse aids.”
Hope in the forecast
Still, optimism exists among some nursing home leaders.
Voepel believes workforce recovery can be achieved much earlier than 2026.
“Absolutely, but we need the federal government to make long-term care a priority,” he said. “We need them to oversee a multi-phased approach with incentives and supports for long-term care, nurse educators or academic resources. With the ever-present ‘silver tsunami’ upon us, we must make a concerted effort nationally to improve the workforce in long term care or the senior network will be inadequate and unable to handle the additional influx of people.”
Parkinson also sees light at the end of the tunnel — provided federal officials provide enough spark.
“Rebuilding the long-term care workforce will not happen by decree,” Parkinson said Monday. “Nursing homes cannot solve this labor crisis on their own. We need policymakers and stakeholders to work together to address the root causes of the staffing challenges in nursing homes and employ a comprehensive set of solutions.”




