
Skilled nursing facilities and assisted living centers treating COVID-19 patients have experienced a 1,064% increase in costs for required personal protective equipment since the deadly virus started its rampage in the U.S.
The rise is even higher (1,084%) for those using nitrile gloves due to vinyl glove shortages or allergies, reported the Society for Healthcare Organization Procurement Professionals.
The group’s analysis attributes the huge price increase to supply-and-demand factors, as well as the increased number of items mandated for safety, and the call for frequent changes.
The independent group said it conducted the analysis to help senior care providers secure federal funding from current and future emergency stimulus packages. Researchers emphasized that findings are not based on estimates but rather actual costs incurred by more than 5,000 SHOPP member facilities serving more than 125,000 seniors nationwide.
“It is mind-blowing,” said Ari Stawis, a SHOPP co-founder, director of professional services and development at Zimmet Health Care, and a former long-term care facility finance director.
“It’s scary as hell because, first, it’s hard to get product, and, second, because of the situation in California,” he told McKnight’s Long-Term Care News. He was referring to a West Coast facility that had to be evacuated Wednesday due to facility staff not showing up for two straight days due to either having contracted the novel coronavirus or fears of it. “If we don’t get product, we don’t have staff show up. And if we can get it, facilities can’t afford it. Unfunded facilities lead to shutting down, and more importantly, not taking care of residents.”
Figures for the analysis were calculated using market pricing plugged into Centers for Disease Control and Prevention guidelines, per new guidance issued by the Centers for Medicare & Medicaid Services’ on April 2, 2020. The new guidelines call for numerous changes of protective equipment for every employee in a covered facility with a COVID-19-positive patient.
As more product comes into the market, prices should start to recede, Stawis acknowledged, but the increase of government and situational requirements, combined with temporarily halted manufacturing in China, created a lethal lag.
“The numbers for what we’re dealing with are just crazy,” Stawis said, noting that pricing changes have been volatile and continue to change daily. “The only way to understand how much of a crisis there is, is to see a report like this.”
Gowns up 2,000%
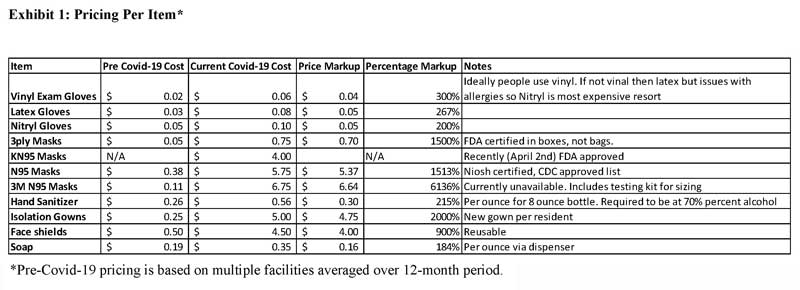
The largest reported price increases have been for isolation gowns (2,000%), N95 masks (1,513%), 3-ply masks (1,500%) and reusable face shields (900%). The most remarkable rise was for 3M N95 masks, which rose from $0.11 to $6.75 each (6,136% increase), though they are currently unavailable, according to SHOPP.
Soap (184%) and nitrile gloves (200%) were the only products of the 11 listed to cost double or less. (See Exhibit 1.)
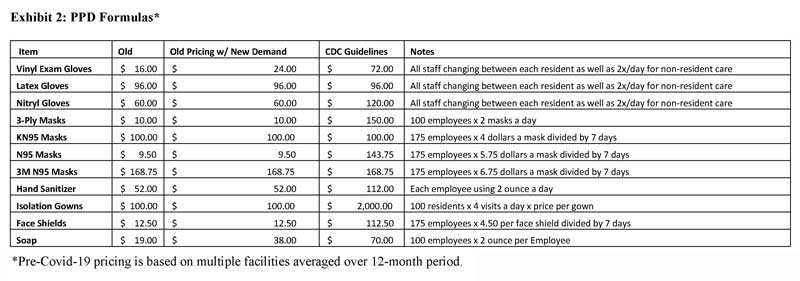
The SHOPP analysis breaks down per-patient-day costs for both pre-COVID and current conditions and requirements. (See Exhibit 2.) Most products would need to be changed multiple times per work shift, with some needing to be refreshed for every new resident encounter.
That’s a far cry from the pre-COVID-19 pricing and requirements, which essentially comprised gloves and soap and water, Stawis said. That amounted to about $0.35 per patient day, which would rise to about $2.36 per patient day when current CDC guidelines are factored in.
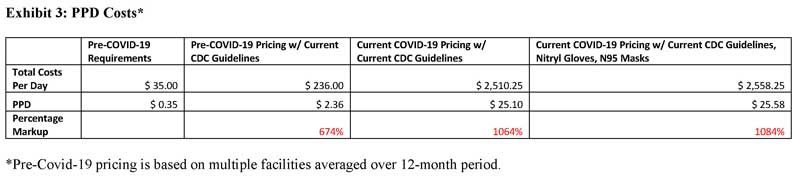
Consider current pricing (as of Monday, April 6) and that figure soars to $25.10 per patient day, producing the 1,064% jump. (See Exhibit 3 above.) Baseline price figures were established by using multiple facilities’ charges over a 12-month period.
The analysis posed circumstances presented by a 100-bed facility multiplied by 30 days for a total of 3,000 census days per month. Assisted living centers use about 25% less PPE than skilled nursing facilities based on different levels of resident interaction, SHOPP estimated. Item prices were reviewed by Faygee Morgenshtern, CEO of People Powered Nursing, and Michael Greenfield, CEO of Prime Source Healthcare Solutions and a co-founder of SHOPP.
The SHOPP study does not take into account labor costs, which also have been subject to larger payouts, organizers pointed out.
U.S. left needing
Stawis explained that when COVID-19 originally broke out in China around the beginning of the year, the U.S. sent a lot of safety products to help. But when the deadly virus landed on American shores a couple of months later, Chinese industry was in the middle of a months-long shutdown and the favor couldn’t be reciprocated.
There hasn’t been enough product since, and distribution vehicles have become unreliable as competition for safety products across the globe heats up. SHOPP nearly had a shipment from overseas to boost U.S. providers recently, but the cargo had a stopover in another country en route, and that country decided to keep the safety products themselves.
The speed and volatility of change is making it difficult to predict the future, Stawis observed. He praised federal officials for allowing advanced Medicare billing and payments so that providers won’t have to dip into their accounts receivable credit lines as quickly. He also recommended that providers ask their vendors for flexible payment terms in these challenging times, and let them know payment terms might have to be extended.
Stawis emphasized the report is not pointing a finger at price gouging for big price increases. Rather, he returns to basic market forces, such as supply and demand, and distribution challenges.
“The products themselves haven’t changed that much, but getting them from the factory to your hands at the nursing home has. Distribution factors, from being held up at customs, to being rerouted, to higher airplane freight charges than in the past,” he said.
SHOPP figures were first given to state association executives starting Tuesday. The Health Care Association of New Jersey, led by Jon Dolan, has been one of the most progressive in pursuing additional support.
SHOPP’s goal was to raise attention to the “dangerous” PPE situation, Stawis said.
“We’re not doing this for one facility or one region,” he noted. “This encompasses the entire nation.”



