
Readmissions are a major problem in U.S. healthcare. Nearly one in five Medicare patients that are discharged from the hospital returns there within 30 days and between 50 percent and 75 percent of those readmissions are considered preventable.1 Medicare pays about $17 billion annually for 2.5 million rehospitalizations of its beneficiaries and other payers spend roughly the same amount every year for all readmissions of non-Medicare patients.2
I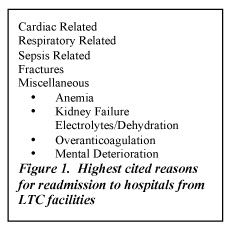 n today’s healthcare world there are increasing economic pressures on preventing readmissions from the Long Term Care (LTC) healthcare setting back to the hospital or other acute care facilities. It is delicate balance between providing the highest level of medical care and today’s economic pressure for profitability. There are also increased regulatory inspections and economic consequences in terms of fines for non-compliance—or tags as they are often called. Additionally, there are quality ramifications on the LTC facility and potential for legal risks from families questioning the level of care for their loved one. Finally, a LTC facility’s reputation can be marred with high admission rates, and hospitals maybe reluctant to refer patients to such a setting.
n today’s healthcare world there are increasing economic pressures on preventing readmissions from the Long Term Care (LTC) healthcare setting back to the hospital or other acute care facilities. It is delicate balance between providing the highest level of medical care and today’s economic pressure for profitability. There are also increased regulatory inspections and economic consequences in terms of fines for non-compliance—or tags as they are often called. Additionally, there are quality ramifications on the LTC facility and potential for legal risks from families questioning the level of care for their loved one. Finally, a LTC facility’s reputation can be marred with high admission rates, and hospitals maybe reluctant to refer patients to such a setting.
A recent published study identified the most frequent health conditions that lead to hospital readmissions (Figure 1).4
The conclusion suggested that LTC facilities find early indicators for such readmissions and develop preemptive plans to prevent and stabilize the patient before readmission is required. Such measures lead to better health and wellbeing of the patient, but end up saving both the individual facilities as well as healthcare in general, substantial costs.
It is generally accepted that 70-85% of all medical decisions are based on clinical laboratory tests, which only account for 1-2% of all healthcare spending —c learly making them a bargain as well as clinically invaluable. They are clearly much less expensive and invasive than medical treatment or clinical sequela downstream.
Furthermore it is also reported that 90% of all patient admits and discharges to and from the hospital are based on the results of a few medical tests. Thus medical test results become more and more valuable in patient management and decision making by clinicians. They are truly the gateway to clinical management of patients.
Yet a recent study concluded that 41% of hospital discharge patients had pending lab results, of which 9.4% were abnormal and could change the patient’s care.5,6 When the test was a blood cultures (which when positive signifies a life-threatening bacterial blood infection) the outcome can be dire.7 Furthermore, these pending results were often omitted from the Joint Commissions required hospital discharge summary, which can impact the patient’s care plan in the next clinical setting—often a long term care facility.8,9,10
The Affordable Care Act 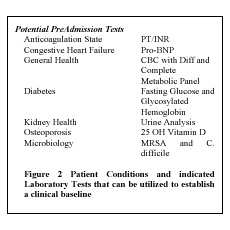 allows for payments to organizations which help manage patients after hospital release and prevent readmission. Hospitals are now taking the lead on managing their discharge patients and thus will have a financial incentive to monitor patients stability in LTC settings to avoid readmissions.
allows for payments to organizations which help manage patients after hospital release and prevent readmission. Hospitals are now taking the lead on managing their discharge patients and thus will have a financial incentive to monitor patients stability in LTC settings to avoid readmissions.
Clearly, both of these new healthcare initiatives lend themselves to keeping patients in a more healthy and stable condition. Medical tests are the key to monitoring the patient’s condition and making early therapeutic decisions.
Even though patients enter the facility with medical records, it is often good to have an intial baseline with the laboratory that will service the patient going forward. This is particularly true for abnormally high Protime/INR tests, which is one of the most significant reasons for LTC readmission back to a hospital.
Baseline Testing
Figure 2 list some suggested tests that would allow for an initial baseline for the patients’ health upon entry to the facility. Such a baseline will allow for monitoring of the patient and early indication of whether the patient’s health is stable, improving or deteriorating.
In addition, clinical result algorithms are being developed by MEDLAB and others that will alert clinicians and LTC staff to potential laboratory results that could lead to readmissions.
In summary, LTC facilities are no longer lone providers in the health of a patient, but rather are a partner in the continuum of care from the initial admission of the patient to a hospital till the patient returns to their home environment or unfortunately get transferred to hospice care. Laboratory results are a key quality indicator for patient stability and can alert LTC facilities to potential patient readmissions and allow for clinical intervention to avoid such situations.
Gary L. Milburn, Ph.D., is the chief technical officer at MEDLAB.
References
1 Stephen F. Jencks, Mark V. Williams, and Eric A. Coleman, “Rehospitalizations Among Patients in the Medicare Fee-for-service Program,” N Engl J Med 2009; 360:1418-1428.
2 Mark Taylor, “The Billion-Dollar U-Turn,” Hospitals & Health Networks, May 2008.
3 Jencks, “Rehospitalization: The Challenge and The Opportunity,” presentation, Integrated Healthcare Association conference, Oct. 2009.
4 Rachel Voss, Rebekah Gardner, Rose Baier,Kristen Butterfield, Susan Lehrman, and Stefan Gravenstein, “The Care Transitions Intervention: Translating from Efficacy to Effectiveness,” Archives of Internal Medicine, vol. 171, no. 14 (July 2011), pp. 1232-1237
5 Roy CL, Poon EG, Karson AS, et al. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005;143:121–8.
6 Walz SE, Smith M, Cox E, Sattin J, Kind J. Pending laboratory tests and the hospital discharge summary in patients discharged to sub-acute care. J Gen Intern Med. 2011 Apr;26(4):393-8. Epub 2010 Nov 30.
7John W. Wilson, MD, William F. Marshall, MD, and Lynn L. Estes, PharmD, RPh Detecting Delayed Microbiology Results After Hospital Discharge: Improving Patient Safety Through an Automated Medical Informatics Tool Mayo Clin Proc. 2011 December; 86(12): 1181–1185.
8 Were MC, Li X, Kesterson J, et al. Adequacy of hospital discharge summaries in documenting tests with pending results and outpatient follow-up providers. J Gen Intern Med. 2009;24:1002-6.
9 The Joint Commission. Standard RC.02.04.01. Available at: http://www.jointcommission.org/. Accessed October 20, 2010.
10 Kripalani S, LeFevre F, Phillips CO, Williams MV, Basaviah P, Baker, DW. Deficits in communication and information transfer between hospital-based and primary care physicians: implications for patient safety and continuity of care. JAMA. 2007;297:831–41.
.





