
Participation in CMS’ Bundled Payments for Care Improvement program is staggering, enhancing the strategic importance of bundled payment activity in your market to your overall strategy and market positioning discussions.
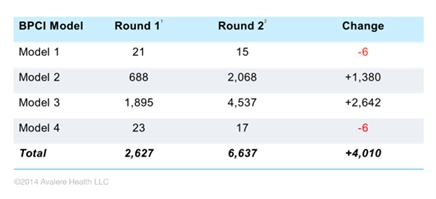
Across the nation, over 6,600 hospitals, physician group practices and post-acute care providers have applied to participate in the BPCI program. While not all of these providers will move forward into the risk-bearing phase of the program in 2015, the level of interest nonetheless indicates that providers across the care continuum are reevaluating how care is delivered under the assumption that they will be financially responsible for patients over the course of an episode of care.
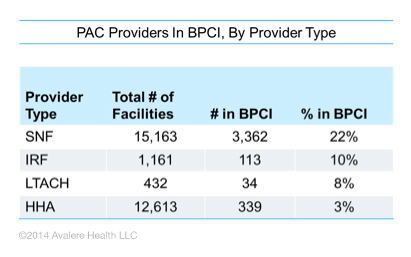
 Skilled nursing facilities are leading the charge, making up over half of all BPCI facility participants. That number jumps to 90% when looking at post-acute care providers only. Even more astounding is that this accounts for 22% of all SNFs nationwide. This participation rate far outpaces adoption of bundled payments by any other PAC setting and does not even include the SNFs who are working with Model 2 and Model 3 participants through gainsharing agreements but who have not applied for the program themselves.
Skilled nursing facilities are leading the charge, making up over half of all BPCI facility participants. That number jumps to 90% when looking at post-acute care providers only. Even more astounding is that this accounts for 22% of all SNFs nationwide. This participation rate far outpaces adoption of bundled payments by any other PAC setting and does not even include the SNFs who are working with Model 2 and Model 3 participants through gainsharing agreements but who have not applied for the program themselves.
 Interestingly, this high level of participation is not driven by the big SNF chains alone. Though many of the largest SNF chains are involved with the BPCI program, the total number of participating facilities owned by these large chains is less than 20% of total SNF participants.
Interestingly, this high level of participation is not driven by the big SNF chains alone. Though many of the largest SNF chains are involved with the BPCI program, the total number of participating facilities owned by these large chains is less than 20% of total SNF participants.
In essence, the BPCI participating SNFs are very representative of the SNF industry as a whole and include a combination of large chains, smaller chains, and free-standing facilities.
The size of the BPCI program and SNF participation rates have implications for all SNFs, regardless if they are formally a part of the program, as there are likely BPCI-participating SNFs in most markets in the U.S. These participating SNFs are highlighting their involvement in the BPCI program in conversations and negotiations with hospitals, integrated delivery networks, and health plans in an effort to become preferred referral partners and to gain additional market share. As more and more providers take on financial accountability for patients, either through the BPCI program, Accountable Care Organizations (ACOs), and managed care contracts, BPCI-participating SNFs can leverage their mutually aligned incentives of managing both care and health care costs for patients over an episode of care. This becomes even more of an imperative for providers in BPCI-saturated markets.
Providers that are not currently participating in BPCI also have opportunities – and depending on the market an imperative – to work with BPCI awardees and evaluate and assess their own strategies and performance. As participants move into the risk-bearing phase of the program, they will be able to take advantage of fraud and abuse waivers that will allow them to gainshare with referral partners. This adds an additional layer of opportunity for BPCI providers to leverage their participation in the program but also opens up possibilities for non-participating providers to engage with up- and downstream partners and to share in both risks and gains achieved through the program.
Non BPCI-participants should consider:
- Participating in gainsharing arrangements or preferred provider partnerships with BPCI participants.
- Obtaining access to Medicare claims data to gain an understanding of key BPCI utilization and performance goals against key market, regional and national benchmarks to inform future value-based purchasing, ACO, and bundled payment opportunities and partnerships
- Initiating care re-design strategies to respond to emerging imperatives to better coordinate care across the continuum, improve quality and improve the patient experience.
The BPCI initiative presents a valuable opportunity for providers to experiment with a new payment system and to catalyze the development of innovative care re-design initiatives. BPCI sets the stage for future bundled payment programs and helps to arm both BPCI-participating and non-participating providers with the structure and tools to be successful in such payment arrangements.
However, SNFs are very early in this process and the ultimate impact of the recent influx of the sector into bundled payments still creates more questions than answers. BPCI participants must decide if they want to remain in the program by April 2015 and must move all the episodes for which they want to bear risk into the program by October 2015. It will be interesting to see how many providers remain in the BPCI program after those deadlines and what challenges and opportunities present themselves to those who are in the program and for those who are not.
Brian Fuller is a director at Avalere Health. Elana Stair is a senior manager at Avalere, advising clients on Medicare post-acute care policy issues focusing on payment delivery system reforms.




